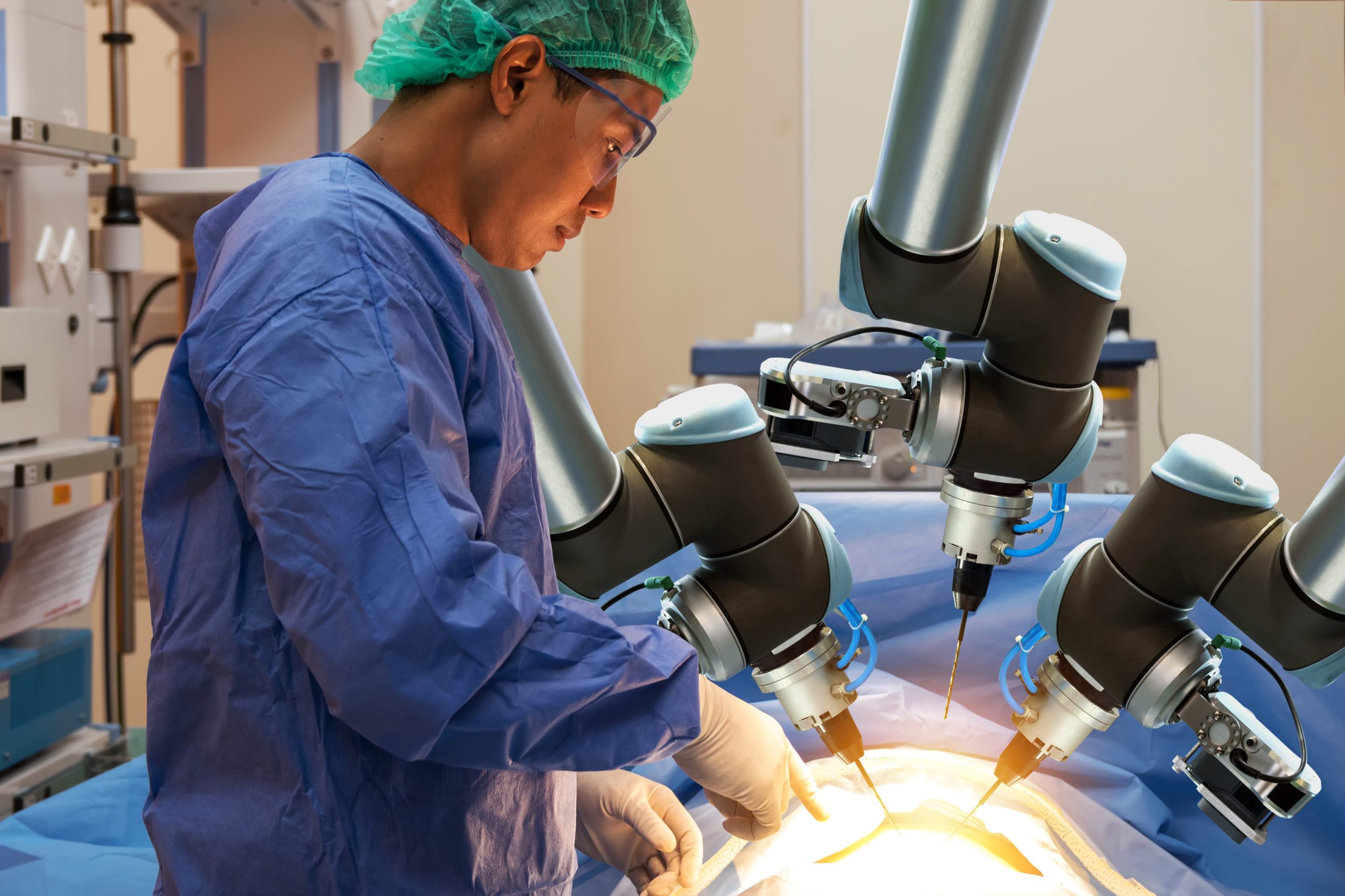
Robot-assisted surgery is becoming increasingly widespread. Its advocates say that it can increase the precision of complicated surgeries, thereby reducing the risk of injury and the time needed to recover. Its critics say that the high costs make it a poor investment for hospitals. But who is right? Are we really ready to put our lives in the hands of machines?
A brief history of robot-assisted surgery
The first robot-assisted surgery took place way back in 1985, when a robotic arm was used to assist in a delicate neurosurgical biopsy. Two years later, the first laparoscopic (keyhole) surgery was performed by the same system. This opened up a world of new opportunities by showing that robotic components could be used for invasive surgeries in a way that made them more precise and less dangerous.
Robot-assisted surgery continued throughout the nineties but the real game changer came in the year 2000 with the introduction of the da Vinci surgical system. This was the first robotic system approved by the FDA for general laparoscopic use and marks the moment that robot-assisted surgery entered the mainstream.
How does it work?
The da Vinci system, now on its second incarnation, the da Vinci Xi, works by allowing a surgeon to carry out their normal work on a much smaller scale. The surgeon sits at a console where they can see an extreme close up of the inside of the patient. The surgeon operates the console using hand and foot pedals and these movements are translated into much smaller movements by the surgical ‘arm’ operating on the patient. This video shows the process in more detail.
The system allows surgery to be more precise. Incisions are smaller and so bleeding and recovery times are reduced. There is also no need for the surgeon to be in the same room, or even in the same country as the patient, meaning that the logistical problems of getting surgeons to operating theatres effectively disappear.
Safety concerns
Robot surgery has taken off in recent years. In 2000 there were just 1000 robot surgeries performed worldwide. By 2012 that number had risen to 450,000. Da Vinci is still the market leader, but a new generation of devices is pushing surgery even further towards automation. The Corindus CorPath 200 is allowing extremely precise heart surgery, while Medtech’s Rosa system is doing the same for neurosurgery.
As with any medical innovation, safety concerns are paramount. In 2013, The Wall Street Journal reported a worrying rise of injuries as a result of robot-assisted surgery. In 2013, there were 50 reports of complications per 100,000 operations, up from 13.3 in 2004. There were also 28 deaths reported following robot-assisted procedures in 2013. The FDA investigated Intuitive, the makers of da Vinci, and issued them a warning for failing to report ‘certain safety changes to its da Vinci robotics system’.
Since then, a number of other incidents have tainted the public perception of robot surgery. Last year Intuitive settled out of court with a patient who alleged the da Vinci system was responsible for complications she suffered after a hysterectomy. It seems wrong to blame the machine in this case though. Robot-assisted surgery is based entirely on the movements and actions of the surgeon. Unless a complication is caused by a mechanical failure, absolute control and absolute responsibility still lies with the operating surgeon.
Failures of robotic surgery systems will always grab headlines. It seems somehow worse to die at the hands of a malfunctioning machine than at the hands of a clumsy surgeon. But is robot-assisted surgery really any more dangerous than human surgery? A detailed 2016 report by the US National Centre for Biotechnology Information analysed FDA data since 2000. There were a total of 144 deaths in this time period which, as one commentator notes, ‘translates to a fraction of one percent for deaths, injuries, and device malfunctions combined.’ It is also impossible to know whether these patients would have died regardless of the type of surgery used. All surgery comes with inherent risks and the statistics show that robot-assisted surgery is extremely safe.
The report also shows that the number of injuries remained steady between 2007 and 2013, despite a huge increase in the number of operations performed in this time period. This suggests that robot-assisted surgery is, in fact, becoming relatively safer, perhaps as training improves and surgeons get used to the equipment.
Is it cost-effective?
The question for the future is not whether robot-assisted surgery will be used, but how it will be implemented. American healthcare is largely private and so it is up to individual hospitals to decide whether robot-assisted surgery is a good investment. In the UK, that decision will have to be made centrally by the government. With the NHS struggling to save money and cut waiting times, robot-assisted surgery seems to be a highly cost-effective solution. Speaking to the Telegraph, Jeremy Russell, CEO of surgical robot manufacturer OR Productivity explained the financial benefits:
‘Robotic systems typically save between 5pc and 10pc of procedure time, sometimes even up to 20pc. With the cost of running an NHS operating theatre around £20 per minute, saving six minutes of time with the robot would pay for itself.’
However, several recent studies disagree with Russell, whose view arguably comes from a place of vested interest. He also fails to mention that the initial cost of the machine is around £1.5 million, meaning that, based on his estimates, around 12,500 surgeries would need to be performed to break even. It is also worth mentioning that his estimates of the cost of running an operating theatre is debatable. This study puts it lower, at around £9.35 a minute.
A study of 23,000 patients who had been treated for kidney conditions found that complication rates between robot-assisted and traditional laparoscopic surgery were much the same, but the robot-assisted surgery cost on average $2600 more and prolonged the operation time. Another study from St James’ University Hospital in Leeds also concluded that robot-assisted surgery currently achieves the same outcomes as traditional surgery but at a higher cost.
It seems that robot-assisted surgery is safe but currently not cost effective. David Jane who led the second study blames the dominance of the da Vinci system for the high costs of robot-assisted surgery:
‘The problem is the market has been dominated by one company who’s had the monopoly on this, and so they’ve been able to charge what they want. As a result, the technology is not cost-effective. The onus is really on other companies to step up and bring in devices and systems that are cost-effective,’
Robot-assisted surgery has the potential to transform healthcare. Making surgery more precise and less invasive is hugely beneficial to patients and, in theory, the reduced recovery times will free up much needed hospital beds. But disruption is needed. It’s time for smaller companies to shake up the industry with new robotic devices. This will either force Intuitive to lower their prices, or will create a cheaper alternative.
To quote Dr Jane, it’s time to ‘throw the gauntlet down to the manufacturers of robotic-assisted technologies.’ That’s where you come in.
Are you the future of healthcare?
If your company is working to improve healthcare using new technology, you should consider applying for an Innovate UK Grant. The latest round of Innovate UK’s Biomedical Catalyst competitions is now open, with two specific streams, namely the Prima and Late Stage awards.
The Prima award invites small and medium sized companies to apply for a share of £4 million for projects looking to develop innovative healthcare products, technologies and processes within disease prevention, earlier and better diagnosis of disease and tailored treatments that change the underlying disease of offer potential cures.
The Late Stage award invites small and medium sized companies to apply for a share of £8 million for projects looking to develop innovative healthcare products, technologies and processes. This includes disease prevention and proactive management of health and chronic conditions, earlier and better detection and diagnosis of disease or tailored treatments that that change the underlying disease of offer potential cures.
The scope of the project within both competitions is fairly wide, covering a number of aspects of healthcare. These include Advanced Therapies, Precision Medicine, Digital Health and Medical Technologies and Devices (improvements in robot-assisted surgery would fall into this final category). Eligible activities in both range from initial human proof-of-concept to phase one and two clinical trials to prototyping, and more.
Because the grants are awarded competitively, your application will need to stand out. You’ll need to convince Innovate UK that your project is more deserving of funding than other similar rival projects. That’s where we can help. We have decades of experience and a proven track record within Innovate UK healthcare applications. We do the heavy lifting so you can focus on your business.